At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is DRESS Syndrome?
Drug rash or reaction with eosinophilia and systemic symptoms (DRESS) syndrome is a medical condition in which a person develops a serious sensitivity to certain prescription medications. It’s also called “drug hypersensitivity syndrome” in some circles. The syndrome isn’t technically an allergy, but it often acts like one, particularly at first. In most cases the first symptom is a spiked fever, usually followed by an itchy rash that quickly spreads over the body. Medical experts aren’t really sure what causes it, though certain classes of drugs are more likely to be triggers than others. Prompt care is usually essential since it can be deadly if it isn’t treated right away. Treatment usually involves stopping the problem drug immediately and, in many cases, flushing its traces out of the body with fluids or steroids.
Initial Symptoms

DRESS syndrome symptoms typically take root anywhere from one to eight weeks after a person starts taking a new drug. Depending on the person’s sensitivity level, it may not take much exposure. Progression does vary from patient to patient, though in most cases symptoms start appearing after at least two weeks of regular dosing.
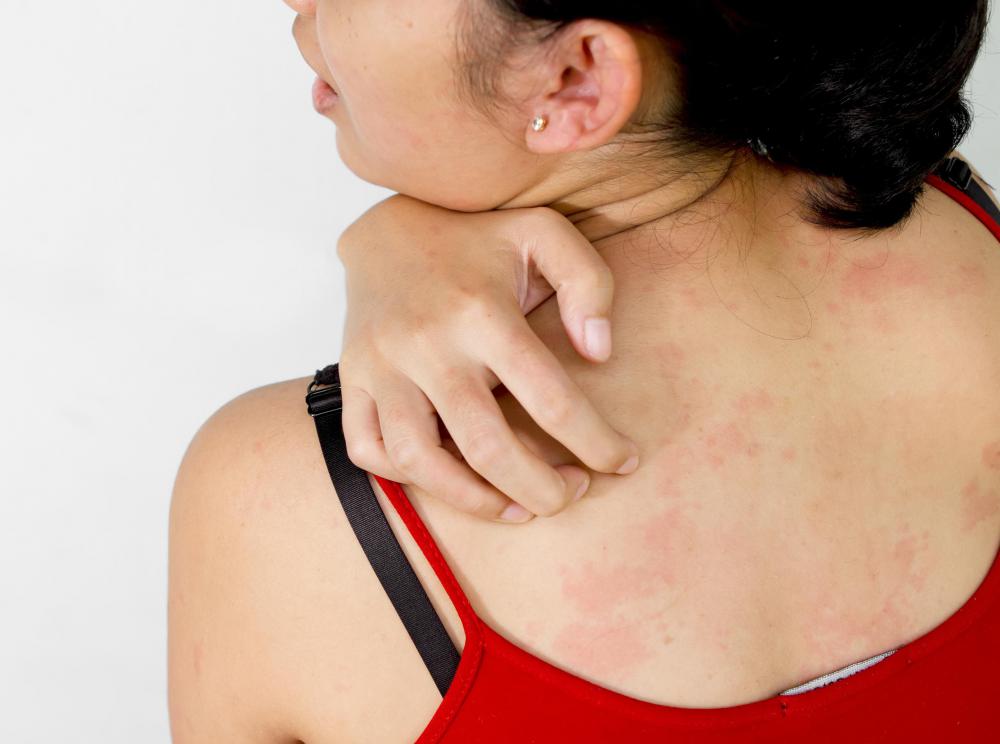
The first thing people usually notice is a high fever. This isn’t always concerning in and of itself, since a lot of things can cause a fever — including in many cases the condition for which the drug is being taken in the first place. In milder cases a raised temperature is one of the only causes, but it’s often accompanied by a widespread skin rash that shifts and moves over the body. The rash is over very long lasting, and won’t usually respond to over the counter ointments or lotions.

If left untreated, the rash can spread and, in serious cases, can progress to exfoliative dermatitis, a skin peeling condition that can be quite painful. Organ damage may soon follow if the condition spreads to the internal systems. Symptoms involving the internal organs can include hepatitis, nephritis, myocarditis, or pneumonitis, all of which can be life threatening.
Main Causes

Researchers and medical experts aren’t entirely sure what causes DRESS syndrome. It’s almost always a problem with the patient’s body rather than the drug, though. Most people who have reactions do so in response to medications that have been rigorously tested and that don’t cause problems for others.
One possible cause is a malfunction in the body’s ability to filter toxins properly through the lymphatic system. This could result in a toxic overload that may result in the condition. Studies conducted to determine possible causes have generally been limited, and have focused mainly on determining the specific types of medications most to blame for the side effects. There is a possible genetic predisposition to this syndrome, and patients who have immediate family members who have suffered from it should alert their healthcare provider before taking any high-risk medications.

Interactions between medications is a common link in DRESS syndrome, and some drugs are more likely to produce it in sensitive people than others. The main categories of prescriptions linked to this condition include the anticonvulsants carbamzepine, phenytoin, and phenobartitone. Specific drugs in these categories include, but are not limited to, atenolol, carbamazepine, dapsone, oxicam NSAIAs, and sulphasalazine. Patients who have experienced symptoms in the past should usually not take these medications if possible and, if essential, should only proceed with the careful guidance of a healthcare provider. p>
How It’s Diagnosed

DRESS syndrome is usually pretty easy to identify through blood tests, and medical providers who suspect it as a potential cause often order a series of blood screens and labs. The syndrome can otherwise be somewhat difficult to diagnose since it often starts out looking like a topical allergy or other type of less threatening sensitivity. For this reason, patients who think that their condition might be linked to a new medication they’ve started need to say so, and also need to be sure to disclose their complete pharmaceutical history when getting treatment.
Treatment Options
Treatment typically starts by immediately stopping all doses of the medication thought to be causing the symptoms. This is best done under the guidance of a healthcare professional, since in most cases people who are taking drugs actually need them for some other condition; experts can often help patients in these situations find other ways of controlling the underlying problem. Keeping the DRESS symptoms under control until the body can properly detoxify itself is often the most important thing. In some patients, systemic steroids have proven beneficial. It is often necessary to continue this sort of detoxifying treatment for several weeks in order to watch for relapse, even after symptoms have ceased.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
I was misdiagnosed as having mono and turned out I had Dress syndrome, I was hospitalized for seven weeks and had multi-organ failure and was intubated due to the severity. I feel that most doctors in the U.S. lack knowledge on DRESS Syndrome. They have yet to figure out which medication caused the initial reaction.
As frustrating as it is, you will eventually get completely over it. It took me three or four months for the rash/hives to completely resolve. Each time I tapered the steroid dose, I would break out into hives and rash for a few days (none of the major initial symptoms).
My doctor decided to taper into half pills and quarter pills at the end, which helped out a lot. It stinks, but you have to be patient. Best of luck to you.
I had DRESS and was misdiagnosed as having a virus. It took me two urgent care visits, one doctor visit, two ER visits and a hospital transfer to get it diagnosed. After a week in the hospital, four days of it in the ICU, they sent me home with steroids, now almost a month later, I just finished the steroids and the rash is coming back! Wish me luck with getting over this.
I lost a workmate to this condition. He had fever, seizures, loss of thought, generalized body rash, and even loss of conscious. He was using tegretol to control seizures.
I was diagnosed with DRESS after taking Bactrim for about four weeks. At first, I thought that I had the flu with a constant fever, aches, and pains. After about two weeks, I broke out in severe rashes all over, had failing liver and kidneys, and gained over 30 pounds in fluid.
Fortunately, the ER that I drove myself to transferred me to a higher level medical facility. Foolishly, I had never related my symptoms to the Bactrim earlier. It took over three months to fully recover.
I was diagnosed with DRESS and Steven's - Johnson Syndrome. I had symptoms of both. I had neurological problems like my legs could not move at first. I could not swallow. The skin on my feet sloughed off, and the lining of my mouth,esophagus, and stomach were like a really raw sore throat. I also experienced the worse imaginable joint pain and skin pain. I wished to die it was so bad. Without excellent physician care and physical therapy, speech therapy and pain control, I would not have made it.
I was hospitalized for two weeks and diagnosed as having Stephen Johnson syndrome. I actually had DRESS. The doctors and staff at the hospital seemed to lack knowledge on this (and SJS).
I was not able to get a dermatology consult, which would have been very beneficial to my case. The offending drug for me was either Cymbalta or carbamazepine.
My son at 17 years of age was diagnosed with DRESS syndrome. At first, the doctors thought it was mono, but after weeks of suffering and another week of hospital stay in an ICU unit, they found it was this DRESS syndrome caused by Lamictal and Bactrin.
If it had been for our persistence in his getting his condition properly diagnosed, the outcome would have been much worse.
Unfortunately, the increase in recent years of hasty diagnoses and drug prescriptions, especially multiple drugs at the same time, has led to more people than ever who have some sort of allergy or reaction to a drug or drugs that they are taking.
Acronyms are so weird. I have no idea why they would think to give the acronym of a woman's piece of clothing to something relating to drug or medicine use. While I imagine it made sense at the time, it's just really odd.
Post your comments