At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Enteral and Parenteral Nutrition?
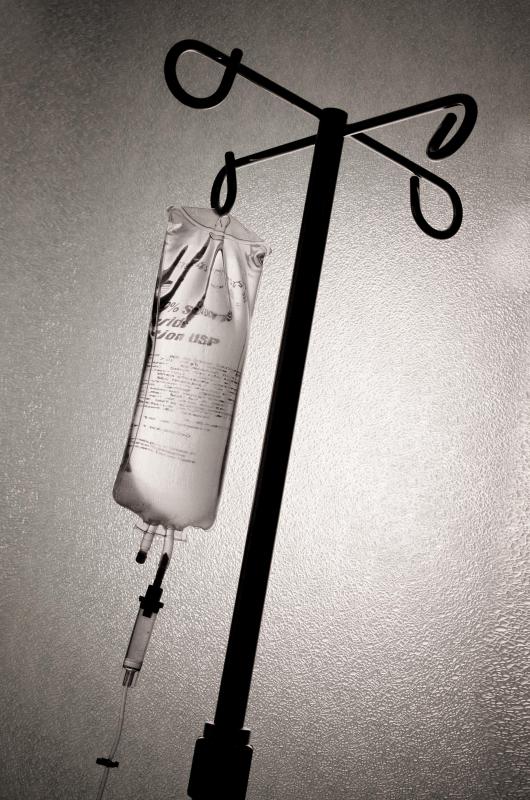
Enteral and parenteral nutrition are two means of delivering nutrition to people who cannot digest food normally. The mechanisms are different, but the overall goal is the same: namely, to provide nutrition and usually also medication directly into patients’ bodies. In most cases the foodstuffs are liquid, and they usually come through a series of tubes and catheters. Enteral feeding delivers liquid nutrition through a catheter inserted directly into the gastrointestinal (GI) tract. Parenteral nutrition, by contrast, provides nutrition intravenously, which means it goes directly into the bloodstream. Entereal feeding usually comes with fewer risks attached, and is often preferred to intravenous feeding when possible.
Why They’re Used

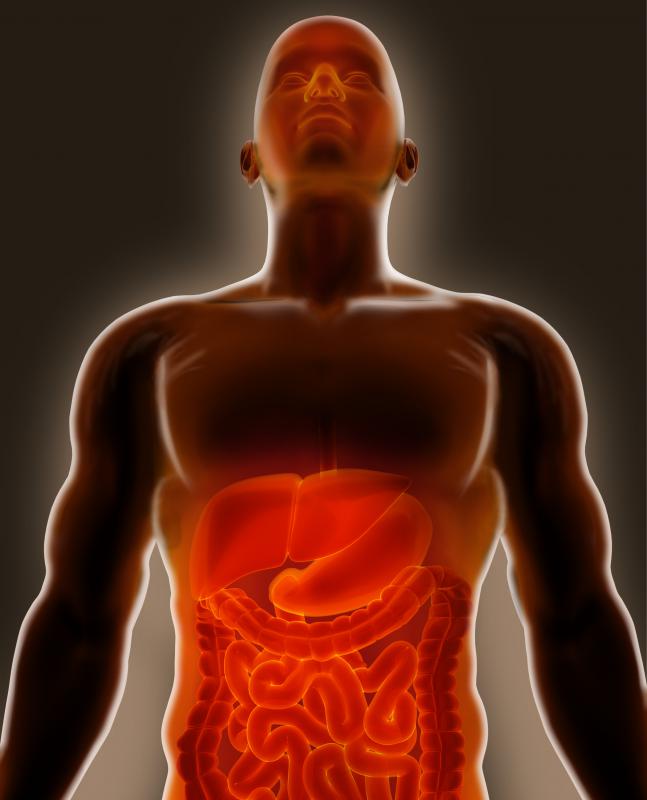
Healthy people digest food through a somewhat complex process that often begins the moment nutrients interact with saliva, and continues as things break down in the stomach, intestines, and colon. The primary organs involved in this process are known collectively as the GI tract and generally include the mouth, where food is taken into the body; the pharynx; the esophagus; the stomach; and the intestines or bowels, which are responsible for the final break-down, absorption, and excretion of food. Things don’t always function the way they should, though. People who have damaged or non-functional GI tracts often need special help getting the right sort of nutrition, and this is where enteral and parenteral nutrition come in.

There are many different reasons why people might need to rely on one of these sorts of systems for food delivery, but invasive illnesses like cancer are some of the most common. In these cases tumors, growths, or required surgeries can close off passageways and make it very difficult for food to be absorbed. A number of other diseases and illnesses can be to blame, too, as can accidents and growth defects. Sometimes the damage is permanent and people have to depend on artificial feeding methods all their lives, but in other cases the tube delivery ends once recovery is complete.
Particulars of Enteral Delivery

Enteral nutrition is usually the easiest to deliver, and all it usually requires is a feeding tube. Nasal tubes tend to be the least invasive, and can be run directly through the patient’s nasal passageway through the esophagus and into the stomach. This bypasses the mouth and throat, but still uses the stomach; as a result it’s only a good choice for people whose stomachs and lower GI tracts work properly.

Nasal tubes cannot be used on patients with obstructions in the esophagus or injuries to the mid-face, however. In these cases, a gastric feeding tube may be surgically placed directly into the stomach, avoiding the nose, mouth, and throat. These procedures are usually performed on patients who have mouth or throat cancer, trauma to the mouth or throat, neurological problems that prevent the patient from swallowing, or patients with severe eating disorders like anorexia nervosa.

When a patient’s stomach is unfit for normal digestion or a catheter, doctors may recommend a jejunostomy tube or “J-tube” instead. The J-tube is a feeding tube that is surgically placed in the jejunum, which is the middle segment of the small intestine. In the digestive tract, the small intestine is positioned after the stomach and is used to break down and absorb food. This can be a good choice for people whose stomachs have problems.
Choosing Parenteral Processes
Enteral feeding isn’t an option for every patient, in particular people who don’t have intestinal capabilities at all. This can be caused by a number of things from post-surgery paralysis of the GI tract to chronic diarrhea or vomiting or, in more serious cases, complete blockages or organ failures. These patients may require total parenteral nutrition (TPN), which delivers nutrition solely through intravenous feeding.
In these circumstances medical professionals typically insert catheters into either the jugular vein; the subclavian vein, below the clavicle; or one of the arm’s large blood vessels. TPN is also recommended for babies with underdeveloped digestive systems, patients with birth defects along the GI tract, people suffering from chronic bowel obstructions, and patients with Crohn’s disease, which is an inflammation of the bowels.
Administration and Duration
In many cases people can return to normal eating after they regain their strength and take on enough calories, but some patients continue to need tube feeding for a long time. Both enteral and parenteral nutrition patients can administer food independently from home in certain chronic cases. These patients often choose to do feedings at night, in order to have their lifestyles be as normal as possible during the day. Feeding operations and care necessarily vary from case to case.
AS FEATURED ON:
AS FEATURED ON:












Discussion Comments
Why does there need to be 2 different syringes? I understand the 2 methods would require very different doses; but why a different syringe?
@anon213472: I am a dietetics student on her way to become a registered dietitian. To answer your question as best as I could, I would say that a feeding tube will prolong his life, but only enough for him to not die of inadequate nutrition (which can cause worse heart problems, more weight loss, etc). It will not give him an abundance of energy. The amounts titrated will only be enough to sustain life. In addition, surgery is only needed if his mouth, nose, and throat are inaccessible. If they aren't, he will he a nasal tube that's placed in 15 minutes without surgery.
In answer to your question, it will just prolong your husband's current life. If he is not eating currently, it will provide additional calories and energy into him. However if he is eating, they could and should offer to provide nutritional supplements for increased calorie intake. You should know this is a surgery that has discomfort and risks associated with it.
I would like to know if this is a last ditch means at sustaining life? My husband is an ESRD, COPD and heart patient! He has lost an enormous amount weight. His doctors have said he has reached zero quality life, he has no interests and exists from one day to the next. He is a permanent resident in a nursing facility. His condition has come to the point that I can no longer care for him at home.
His dialysis clinic wants to try this procedure in order to give him more energy and maybe put some weight on. I want someone who will answer my questions honestly.
Is this something that will give him quality life or just prolong the life he currently has? Someone please answer my questions honestly! I am tired of watching him suffer.
@healthnwell--This can be a hard time for the patient and the family, we had someone in our family that needed parenteral nutrition for quite some time. I hope your friend feels better soon. We found great information and support by contacting the Oley Foundation and the patient information section of the American Society for Enteral and Parenteral Nutrition (A.S.P.E.N.). They both have extensive websites. Good Luck!
A friend of our family has had to have enteral feeding support for quite a while now; does anyone know of a website where they can look for educational and emotional support? Thanks for any info!
Great information and easy to understand. Thanks.
Post your comments